Enlargement countries - health statistics
Data extracted in April 2023.
Planned article update: June 2024.
Highlights
In 2021, public expenditure on health relative to GDP was lower in all the Western Balkans and Türkiye than in the EU.
There were more discharges of in-patients from hospitals, relative to population size, in the EU than in any of the Western Balkans in 2021.
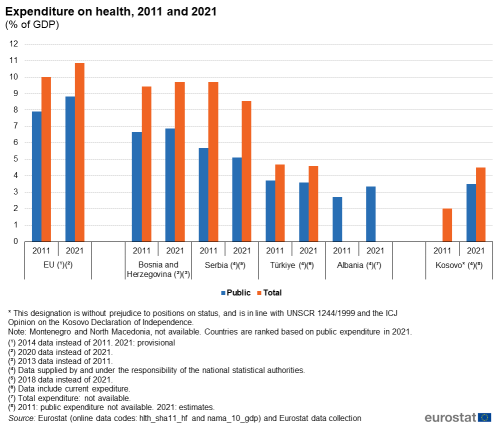
Public expenditure on health, 2011 and 2021 (% of GDP)
This article is part of an online publication and provides information on a range of health statistics for the Western Balkans and Türkiye and compares this with the corresponding data for the European Union (EU). Within this region, Bosnia and Herzegovina, Montenegro, North Macedonia, Albania, Serbia and Türkiye are candidate countries, while Kosovo* has the status of potential candidate.
Data for Georgia, Moldova and Ukraine, granted candidate status or European perspective by the European Council in June 2022, are not included in this article; Statistics Explained articles on the European Neighbourhood Policy-East countries are available here.
Health statistics measure both objective and subjective aspects of people's health. They cover key indicators on the functioning of the health care systems and health and safety at work. Statistics on healthcare expenditure and financing may be used to evaluate how a healthcare system responds to the challenge of universal access to quality healthcare. Financial resources within the healthcare sector are measured, as are the allocation of these resources between healthcare activities, such as preventive and curative care, or groups of healthcare providers, for example, hospitals and ambulatory centres.
This article gives an overview of health developments in the Western Balkans and Türkiye and in the EU, presenting an analysis of health expenditure, health resources, hospital discharges, healthcare personnel and health status.
*This designation is without prejudice to positions on status, and is in line with UNSCR 1244/1999 and the ICJ Opinion on the Kosovo Declaration of Independence.
Full article
Public expenditure on health
Public and total health expenditure as a percentage of gross domestic product (GDP) provide measures of how much resources are invested in the health of the population. In Figure 1, data on these ratios for 2021 (or the most recent year available) is compared to data for 2011 for the Western Balkans and Türkiye, where available.
In Bosnia and Herzegovina expenditure on health remained largely unchanged as a percentage of GDP over the decade, with the share of public health expenditure slightly up from 6.7 % of GDP in 2013 to 6.9 % in 2020 (the most recent year available) and total expenditure on health up from 9.4 % to 9.7 %. Serbia’s public health expenditure amounted to 5.1 % of GDP in 2018 (the most recent year available). In comparison, it stood at 5.7 % of GDP in 2011. Total health expenditure also diminished as a share of GDP over this period, from 9.7 % of GDP in 2011 to 8.6 % in 2018. In Türkiye, the ratios fell more moderately between 2011 and 2021. While public expenditure on health decreased from 3.7 % of GDP to 3.6 %, total expenditure on health fell from 4.7 % of GDP to 4.6 %. For Albania, data are only available for public health expenditure. This provisionally increased as a share of GDP from 2.7 % in 2011 to 3.4 % in 2021.
In Kosovo, public expenditure on health was estimated at 3.5 % of GDP in 2021 and total expenditure on health increased from 2.0 % of GDP in 2011 to 4.5 % in 2021; data on public expenditures are not available for 2011.
In 2021 public expenditure on health in the EU was estimated at 8.8 % of GDP, while total expenditure amounted to 10.9 %. This was higher than in all the Western Balkans and Türkiye. In 2021, expenditure on health and the share of public health expenditure increased by 0.9 percentage points each compared to 2011.
Note that the developments described reflect changes both in health expenditure and in GDP; a falling health expenditure relative to GDP does not necessarily mean that the absolute level of health expenditure is lower than before. Alternatively, it may be an indication that health expenditures are not rising as rapidly as GDP.
(% of GDP)
Source: Eurostat (hlth_sha11_hf) and (nama_10_gdp) and Eurostat data collection
Healthcare resources
Figure 2 presents data on hospital discharges of in-patients, an indicator of the level of healthcare activity in hospitals. A hospital discharge occurs when a patient is formally released after an episode of care: discharge may result from the end of the treatment; a decision by the patient to sign out against medical advice; the patient’s transfer to another healthcare institution; or because of death. Trends in hospital discharges per 100 000 inhabitants over time can be affected by a number of factors: the level of hospital capacity and activity; the average length of the treatments carried out in the hospitals; the introduction of new medical treatments in the hospitals; and in-patient treatments being replaced by out-patient treatments (which are normally less expensive) for all or for a part of the total treatment period. For EU countries, including the estimated EU total, 2020 is the latest year for which data are available; it is also the year when the data began to be affected by the Covid-19 pandemic. At the time of writing, 2021 data were available for all Western Balkans and Türkiye.
Türkiye had 13 918 hospital discharges per 100 000 inhabitants in 2021. This was the highest among the Western Balkans and Türkiye. Between 2011 and 2021, the number of discharges relative to the population decreased by 10 %; however, please note that there is a break in series and that the definition differs from the standard definition. Montenegro had the next highest level of hospital discharges per 100 000 inhabitants in 2021, at 12 394. This represented an increase of 3 % compared to 2011. In Serbia, the hospital discharges stood at 12 036 per 100 000 inhabitants in 2021, which was 23 % lower than in 2011.
There were 8 670 hospital discharges per 100 000 inhabitants in Albania in 2021, the lowest ratio of in-patient discharges relative to population size in the region, it was 4 % down compared to 2011. Kosovo registered 8 815 hospital discharges per 100 000 inhabitants in 2021. Data for 2011 were not available for Kosovo. Data was not available for either year for North Macedonia and Bosnia and Herzegovina.
In 2020, the most recent year available for most of the EU Member States, there were an estimated 13 153 hospital discharges per 100 000 inhabitants across the EU. This number has decreased by 10 % since 2011. Figure 2 also shows the two EU Member States with the highest and lowest number of hospital discharges per 100 000 population in 2020 (2021 data not yet available). The highest value among the EU Member States was recorded in Bulgaria, at 28 250 discharges per 100 000 inhabitants in 2020, an increase of 6 % from 2011 to 2020 and much higher than for any of the Western Balkans and Türkiye. The lowest rate was registered in Portugal, with 7 393 hospital discharges per 100 000 inhabitants in 2020, a decrease of 14 % compared to 2011.
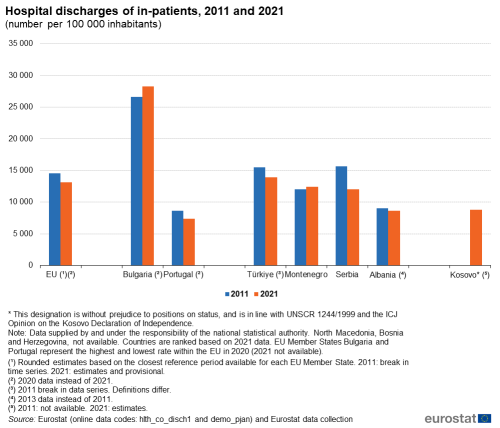
(number per 100 000 inhabitants)
Source: Eurostat (hlth_co_disch1) and (demo_pjan) and Eurostat data collection
Figure 3 provides information on healthcare personnel. Physicians need to possess a degree in medicine and are licensed to provide treatment to patients, including: giving advice, conducting medical examinations and making diagnoses; applying preventive medical methods; prescribing medication and treating diagnosed illnesses; giving specialised medical or surgical treatment.
Nursing professionals typically provide services to patients in hospitals, ambulatory care and patients’ homes: nurses assume responsibility for the planning and management of patient care, including the supervision of other healthcare workers, working autonomously or in teams with medical doctors and others in the application of preventive and curative care.
Midwives plan, manage, provide and evaluate care services during pregnancy and after childbirth, providing delivery care for reducing health risks to women and new-born children; they may work autonomously or in teams with other healthcare providers.
Among those in the Western Balkans and Türkiye for which data are available, the highest numbers of physicians relative to population size in 2021 were recorded in North Macedonia (2020 data) with 301.4, Serbia with 301.3 and Montenegro with 280.7 physicians per 100 000 inhabitants. Bosnia and Herzegovina followed with 232.2 physicians per 100 000 inhabitants (2020 data instead of 2021). However, the data for Bosnia and Herzegovina cover only professionals working in public institutions and are therefore not directly comparable with the other Western Balkans and Türkiye. Türkiye recorded 206.0 physicians per 100 000 inhabitants (2020 data instead of 2021), covering only professionally active physicians. Kosovo followed far behind, estimating 9.1 physicians per 100 000 inhabitants in 2021.
Türkiye recorded the highest rate of dentists in the region, with 47.1 per 100 000 inhabitants, covering only the professionally active. Serbia followed with 24.4 dentists per 100 000 inhabitants. Bosnia and Herzegovina (2020 data) recorded 23.5, counting only those working in public institutions, and Kosovo estimated 22.8 dentists per 100 000 inhabitants in 2021. Montenegro reported a much lower level of dentist coverage in 2021, just like in the preceding years, corresponding to 6.0 dentists per 100 000 inhabitants.
The coverage of pharmacists did not vary as much throughout the region as the coverage of some other categories of health personnel. Türkiye had the highest coverage with 43.9 pharmacists per 100 000 inhabitants, while the lowest coverage was seen in Bosnia and Herzegovina (2020 data) with 15.3. Between these, Kosovo recorded 29.7, Montenegro 23.7 and Serbia 15.7 pharmacists per 100 000 inhabitants in 2021.
Bosnia and Herzegovina registered 612.2 nursing professionals per 100 000 inhabitants (2020 data instead of 2021), the highest in the region, only covering nurses in public institutions. Kosovo with 552.6 and Montenegro with 533.4 nursing professionals per 100 000 inhabitants also reported coverage above 500 in 2021. Much lower ratios were recorded in Türkiye with 274.5 professionally active nurses (2019 data instead of 2021) and Serbia with 101.2 per 100 000 inhabitants.
The ratio of midwives to population was by far the highest in Türkiye, with 68.4 professionally active midwives per 100 000 inhabitants (2019 data instead of 2021). In 2021, Montenegro had 42.2 and Bosnia and Herzegovina 29.4 midwives (2020 data instead of 2021) per 100 000 inhabitants, respectively, with Bosnia and Herzegovina only registering those working in public institutions. In Serbia and Kosovo, coverage by midwives was substantially lower, with ratios of respectively 16.3 and 4.9 per 100 000 inhabitants in 2021.
In comparison, in the EU there were an estimated 391.4 physicians (2020 data), 57.6 dentists, 82.6 pharmacists, 502.4 nursing professionals and 25.1 midwives per 100 000 inhabitants in 2021; the estimates are based on the closest reference period available for each EU Member State. The Member State with the highest coverage of physicians, Greece, had 618.5 physicians per 100 000 inhabitants in 2020, while the lowest coverage registered was 313.3 for Hungary (2020 data instead of 2021).
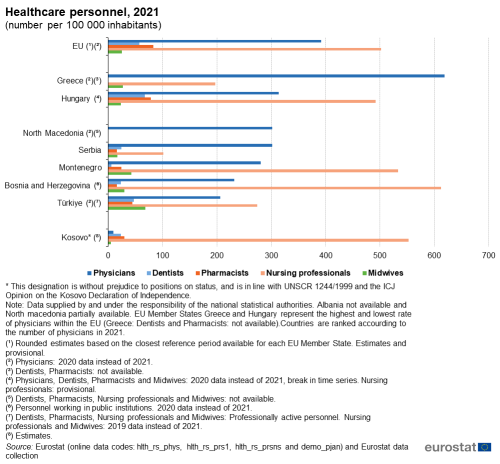
(number per 100 000 inhabitants)
Source: Eurostat (hlth_rs_phys), (hlth_rs_prs1), (hlth_rs_prsns) and (demo_pjan) and Eurostat data collection
Figure 4 illustrates the number of midwives per 1 000 live births, which takes account of the birth rate. Most of the Western Balkans and Türkiye for which data are available for both 2011 and 2021 showed a decrease in this ratio over the decade. Türkiye had the highest ratio of midwives, at 68.4 professionally active midwives per 1 000 live births, down from 69.5 in 2011. Montenegro was the only country in the region that recorded an increase in the coverage of midwives to assist at birth, rising from 37.9 midwives per 1 000 live births in 2011 to 42.2 in 2020 (latest data). In Bosnia and Herzegovina there were 29.4 midwives working in public institutions per 1 000 live births in 2020 (2021 data not available), compared to 34.7 in 2011. Serbia recorded 18.1 midwives per 1 000 live births in 2021, there is no 2011 data for Serbia. In Kosovo, there were 4.9 midwives per 1 000 live births in 2021, data for Kosovo for 2011 are not available.
For the EU, the ratio of midwives per 1 000 live births stood at 36.1 in 2021 (or in the closest reference period available for each EU Member State) up from 32.5 in 2011.
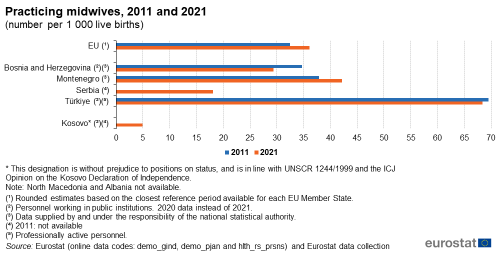
(number per 1 000 live births)
Source: Eurostat (demo_gind), (demo_pjan) and (hlth_rs_prsns) and Eurostat data collection
Health status
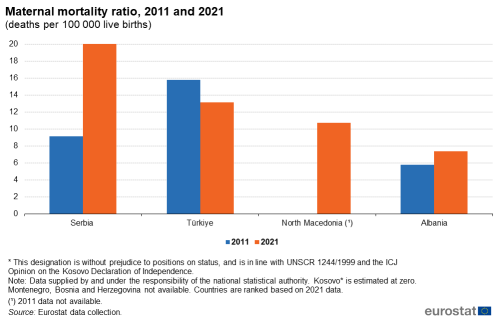
This section examines the maternal mortality rate and the incidence of two diseases, tuberculosis and hepatitis B. The maternal mortality rate is defined by the United Nations as the annual number of female deaths from any cause related to or aggravated by pregnancy or its management (excluding accidental or incidental causes) during pregnancy and childbirth or within 42 days of the termination of pregnancy, irrespective of the duration/place of pregnancy. It is expressed as a ratio per 100 000 live births. Deaths related to pregnancy and childbirth are very rare and so, particularly within smaller populations, even a difference of two or three deaths between years can result in relatively large percentage changes.
Data supplied by and under the responsibility of the national statistical authority are available on the maternal mortality ratio for three of the Western Balkans and Türkiye. It is presented in Figure 5 for 2011 and 2021. Serbia recorded a substantial growth, from 9.1 in 2011 to 22.5 deaths per 100 000 live births in 2021. The rate in Türkiye in 2021 was 13.1 deaths per 100 000 live births, a decrease from the 2011 figure of 15.8. North Macedonia recorded a maternity mortality rate of 10.7 in 2021, but 2011 data for comparison is not available. In Albania, the maternal mortality ratio increased from 5.8 deaths per 100 000 live births in 2010 to 7.3 in 2021.
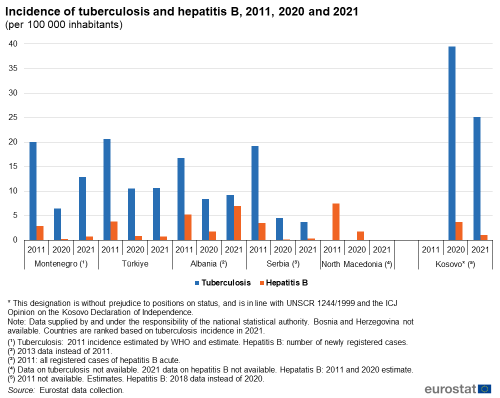
In 2021, the incidence of tuberculosis among Western Balkans and Türkiye – presented in Figure 6 – was highest in Kosovo, at 25.1 cases per 100 000 inhabitants (2011 data not available). This was far higher than elsewhere in the region, as the next highest incidence rate was recorded in Montenegro at 12.9; however, this was considerably lower than in 2011, when the incidence of tuberculosis in Montenegro was 20.0 per 100 000 inhabitants. In Türkiye, the incidence stood at 10.7 in 2021, which is a little bit more than half of the 20.6 per 100 000 inhabitants recorded in 2011. Both Albania and Serbia recorded strong declines in their tuberculosis incidences over the period 2011-2021. In 2021, Albania registered 9.3 cases per 100 000 inhabitants — in 2011, the incidence was 16.8. Similarly, in Serbia the incidence of tuberculosis fell from 19.2 cases per 100 000 inhabitants in 2011 to 3.8 in 2021. Data on the incidences of tuberculosis are not available for North Macedonia and for Bosnia and Herzegovina.
For all of the Western Balkans and Türkiye for which such data are available, there was a sharp decline in the incidence of hepatitis B from 2019 to 2020 due to prevention measures put in place in connection with the Covid-19 pandemic that may have limited the spread also of other transmittable diseases such as tuberculosis and hepatitis. In 2021, three out of four countries for which data are available showed growth in their incidences of hepatitis B in comparison to the previous year but the levels of the disease in most of them are still lower of those in 2011.
Among the Western Balkans and Türkiye, Albania registered the highest incidence of hepatitis B in 2021, at 7.0 newly registered cases per 100 000 inhabitants. The incidences reported for 2021 by other countries were less than 1 case of hepatitis B per 100 000 inhabitants, which were reported by Serbia (0.4), Montenegro (0.8) and Türkiye (0.8). For North Macedonia, the hepatitis B incidence was estimated at 1.8 in 2020 down from 7.5 in 2011; for Kosovo, 2011 data are not available but in 2021 there were 1.1 cases of hepatitis B per 100 000 inhabitants, less than one third of 2020 cases.
For Türkiye, the most recent reported incidence of hepatitis B was 0.8, which was down from 3.8 in 2011. Montenegro and Serbia (all registered cases of acute hepatitis B) had similar outcomes in 2021, with 0.8 and 0.4 cases per 100 000 inhabitants, respectively, down from 2.9 for Montenegro and 3.5 for Serbia in 2011.
Source data for tables and graphs
Data sources
The enlargement countries are expected to increase the volume and quality of their data progressively, and to transmit these data to Eurostat and the wider ESS in the context of the EU accession process. The final objective of the EU in relation to official statistics is to obtain harmonised, high-quality data that conforms to both European and international standards. More details on the statistical aspects of the accession process can be found in the article Enlargement policy and statistical cooperation.
The enlargement countries are not at the same level of development and are progressing towards an efficient and modern statistical system at different speeds. In a number of areas, candidate countries (and sometimes also potential candidates) are in a position to provide harmonised data in accordance with the EU acquis with respect to methodology, classifications and procedures for data collection and the principles of official statistics as laid down in the European statistics Code of Practice. In these cases, the candidate countries (and potential candidates) concerned report their data to Eurostat following the same procedures and under the same quality criteria as the EU Member States and the EFTA countries. Data from the enlargement countries that meet these quality requirements are published along with data for EU Member States and EFTA countries.
In addition, the enlargement countries provide data for a wide range of indicators for which they do not yet fully adhere to the quality requirements specified in the EU acquis and the methodology, classifications and procedures for data collection specified in the relevant Regulations, Directives and other legal documents. These data are collected on an annual basis through a questionnaire sent by Eurostat to the candidate countries or potential candidates. A network of contacts has been established for updating these questionnaires, generally within the national statistical offices, but potentially including representatives of other data-producing organisations (for example, central banks or government ministries). This annual exercise also provides an opportunity to provide methodological recommendations to the enlargement countries.
In December 2008, the European Parliament and the Council adopted Regulation (EC) No 1338/2008 on Community statistics on public health and health and safety at work. It was designed to ensure that health statistics provide adequate information for all EU Member States to monitor Community actions in the field of public health and health and safety at work. It lists five domains for which implementing regulations specifying (in detail) the list of variables and methodological aspects were to be developed, including:
- health status and health determinants: Regulation (EU) No 141/2013 on European Health Interview Survey;
- health care: as covered by Regulation (EU) No 141/2013 and Regulation (EU) 2015/359 on statistics on healthcare expenditure and financing;
- causes of death: Regulation (EU) No 328/2011 on statistics on causes of death;
- accidents at work: Regulation (EU) No 349/2011 on statistics on accidents at work;
- occupational diseases and other work-related health problems and illnesses: Commission Communication COM(2021) 323 final EU strategic framework on health and safety at work 2021-2027 — Occupational safety and health in a changing world of work
Tables in this article use the following notation:
| Value in italics | data value is forecasted, provisional or estimated and is therefore likely to change; |
| : | not available, confidential or unreliable value. |
Context
EU policies seek to improve and foster health in the European Union; protect people in the European Union from serious cross-border threats to health; improve medicinal products, medical devices and crisis-relevant products; and strengthen health systems. The Covid-19 pandemic has a major impact on patients, medical and healthcare staff, and health systems in Europe. The 2021-2027 EU4Health programme will go beyond crisis response to address healthcare systems’ resilience. Established by Regulation (EU) 2021/522 establishing a Programme for the Union’s action in the field of health (‘EU4Health Programme’) for the period 2021-2027, it will provide funding to eligible entities, health organisations and NGOs from EU countries and to non-EU countries associated to the programme.
Health statistics are used to monitor the EU’s health strategy as well as their contribution to the sustainable development goals (SDGs). These statistics have a key role to support the development of evidence-based policies both nationally and within the EU. They also serve as a basis for calculating indicators to monitor some aspects of social protection and social inclusion and a set of indicators known as the European core health indicators (ECHI).
Diseases are classified according to the International Statistical Classification of Diseases (ICD) of the World Health Organization (WHO). Eurostat's Cause of death (COD) statistics build on standards set out in the ICD. Since reference year 2014, all countries reporting for Eurostat's COD statistics follow the ICD classification in its tenth revision (ICD-10).
While basic principles and institutional frameworks for producing statistics are already in place, the Western Balkans and Türkiye are expected to increase progressively the volume and quality of their data and to transmit these data to Eurostat in the context of the EU enlargement process. EU standards in the field of statistics require the existence of a statistical infrastructure based on principles such as professional independence, impartiality, relevance, confidentiality of individual data and easy access to official statistics; they cover methodology, classifications and standards for production.
Eurostat has the responsibility to ensure that statistical production of the Western Balkans and Türkiye complies with the EU acquis in the field of statistics. To do so, Eurostat supports the national statistical offices and other producers of official statistics through a range of initiatives, such as pilot surveys, training courses, traineeships, study visits, workshops and seminars, and participation in meetings within the European Statistical System (ESS). The ultimate goal is the provision of harmonised, high-quality data that conforms to European and international standards.
Key Community legislation regarding health statistics is listed under 'Legislation' on the dedicated section on 'Health statistics' on Eurostat's website.
Additional information on statistical cooperation with the enlargement countries is provided here.
Direct access to
Other articles
- Enlargement countries — statistical overview — online publication
- Statistical cooperation — online publication
- Healthcare_expenditure_statistics
- Hospital_discharges_and_length_of_stay_statistics
Publications
- Statistical books/pocketbooks
- Key figures on enlargement countries — 2019 edition
- Key figures on enlargement countries — 2017 edition
- Key figures on the enlargement countries — 2014 edition
- Factsheets
- Basic figures on the candidate countries and potential candidates — Factsheets — 2023 edition
- Basic figures on Western Balkans and Türkiye — Factsheets — 2022 edition
- Basic figures on enlargement countries — Factsheets — 2021 edition
- Leaflets
- Basic figures on enlargement countries — 2020 edition
- Basic figures on enlargement countries — 2019 edition
- Basic figures on enlargement countries — 2018 edition
- Basic figures on enlargement countries — 2016 edition
Database
- Health (hlth), see:
- Health status (hlth_state)
- Health determinants (hlth_det)
- Health care (hlth_care)
- Health care expenditure (SHA 2011) (hlth_sha11)
- Health care resources (hlth_res)
- Health care activities (hlth_act)
- Disability (hlth_dsb)
- Causes of death (hlth_cdeath)
- Health and safety at work (hsw)
Dedicated section
Methodology
- Western Balkans and Türkiye (ESMS metadata file — cpc_esms)
- Implementing Regulations:
- Regulation (EU) 328/2011 on statistics on causes of death;
- Regulation (EU) 349/2011 on statistics on accidents at work;
- Regulation (EU) 141/2013 on statistics based on the European Health Interview Survey;
- Regulation (EU) 2015/359 on production of statistics on healthcare expenditure (for the reference period 2014–2020);
- Regulation (EU) 2021/1901 om production of statistics on healthcare expenditure (with 2021 as the first reference year).
External links
- European Commission — European Neighbourhood Policy and Enlargement Negotiations
- European Commission — Health and Food Safety
- EU4Health Programme — a vision for a healthier European Union
- World Health Organization (WHO): International Statistical Classification of Diseases and Related Health Problems — 10th Revision (ICD-10)