Self-perceived health statistics
Data extracted in: November 2023.
Planned article update: December 2024.
Highlights
More than two thirds (67.8 %) of people in the EU perceived their health as very good or good in 2022.
Self-perceived gender health gap in the EU in 2022: males tended to rate their health better than females.
More than one third (36.1 %) of people in the EU reported having a long-standing (chronic) health problem in 2022.
This article presents an overview of the self-reported health status of European Union (EU) population. The data come from EU statistics on income and living conditions (EU-SILC) and relate to the 2022 reference year; they cover persons aged 16 years or over. These data focus on two key indicators describing the levels and distribution of health status:
- self-perceived health gives an overall assessment by respondents of their health in general;
- chronic morbidity assesses the presence of a long-standing illness or health problem.
This article is one of a set of statistical articles on health status which forms part of Chapter 1 in an online publication, Health in the European Union – facts and figures.
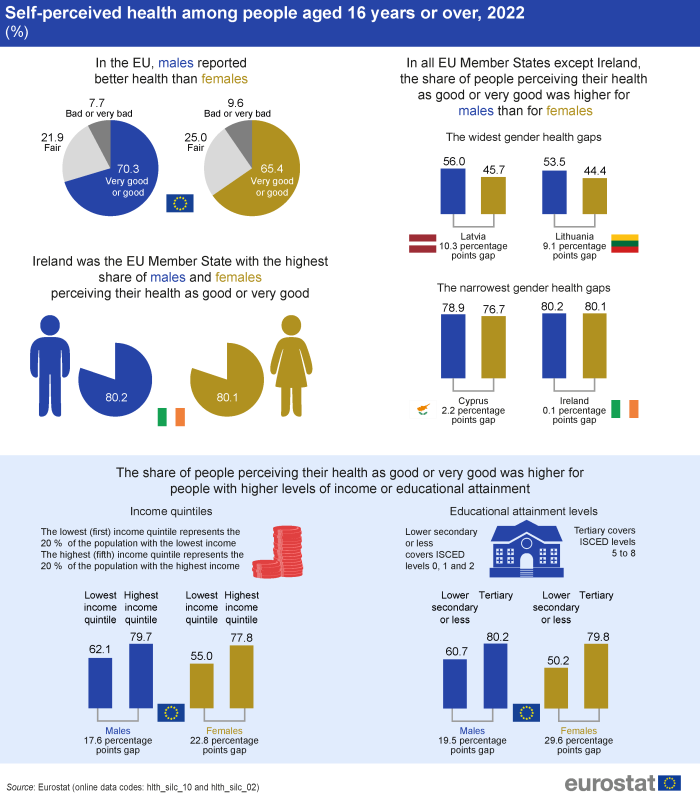
(%)
Source: Eurostat (hlth_silc_10) and (hlth_silc_02)
Full article
Self-perceived health
More than two thirds of people in the EU perceive their health as very good or good in 2022
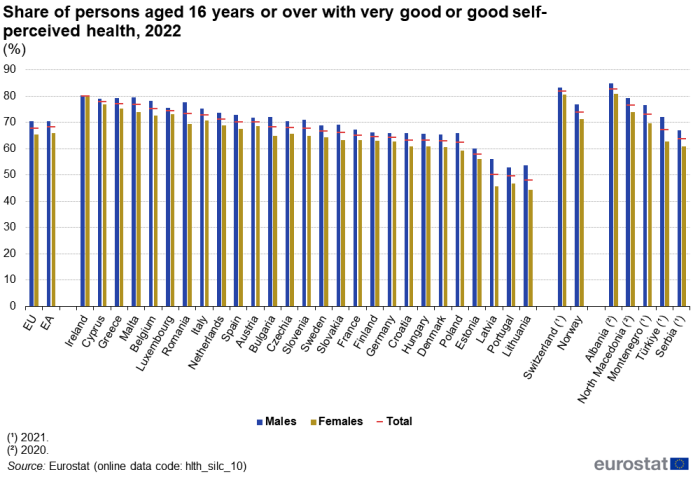
(%)
Source: Eurostat (hlth_silc_10)
In the EU, 67.8 % of the population aged 16 years or over perceived their health as very good or good in 2022 – see Figure 1. Across the EU Member States, the share of people who perceived their health as very good or good ranged from less than half in Lithuania (48.1 %) and Portugal (49.5 %) to more than three quarters in Belgium (75.3 %), Malta (76.7 %), Greece (77.2 %), Cyprus (77.8 %) and Ireland (80.1 %). Among the non-EU countries for which data are presented in Figure 1, Switzerland (2021 data), Albania (2020 data) and North Macedonia (2020 data) also recorded shares above three quarters.
Self-perceived gender health gap: males tend to rate their health better than females
In 2022, the gender health gap in the EU was 4.9 percentage points, as 70.3 % of males aged 16 years or over rated their health as very good or good compared with 65.4 % of females of the same age. Across all of the EU Member States, males were more likely than females to rate their health as very good or good – see Figure 1 and Table 1. The largest gender health gaps in percentage point terms were recorded in Latvia (10.3 percentage points), Lithuania (9.1 percentage points) and Romania (8.4 percentage points). By contrast, there was almost no difference between the sexes in terms of the gender health gap in Ireland, as the share of males that rated their health as very good or good was 0.1 percentage points higher than that for females.
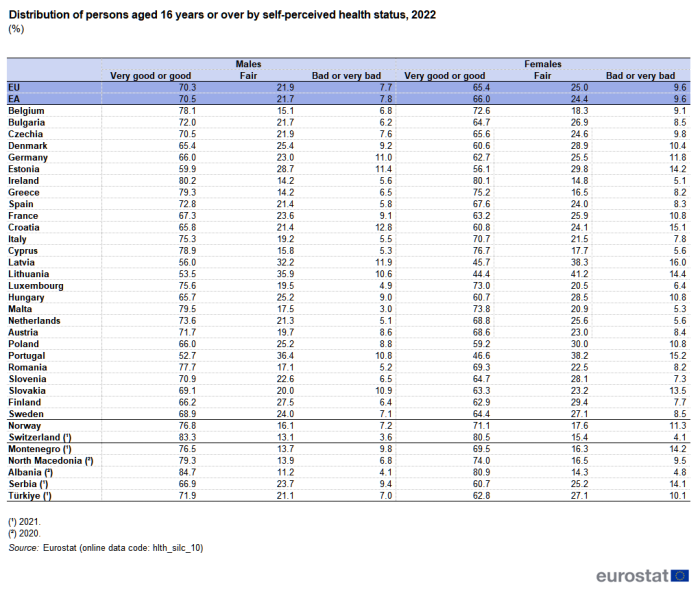
(%)
Source: Eurostat (hlth_silc_10)
Conversely, when focusing on the population that rated their health as bad or very bad, the shares for women were generally higher than those for men. In the EU, 9.6 % of females and 7.7 % of males regarded their health as bad or very bad in 2022.
Negative perception of health increased with age, as did the gender health gap
Self-perceived health also has a distinct age pattern as fewer people tended to rate their health as being very good or good in higher age groups than in lower age groups, while the share reporting bad or very bad health increased with age – see Figure 2. Similarly, the share of persons reporting that their health was fair generally increased with age, although for females there was a small decrease in the share reporting that their health was fair between the age groups 75–84 years and 85 years and over.
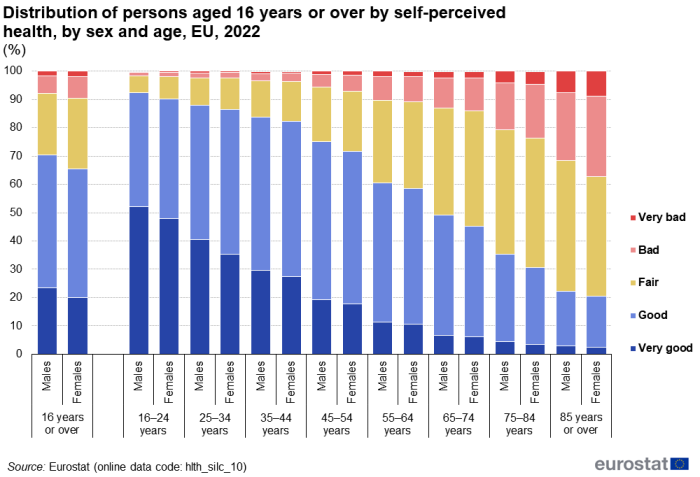
(%)
Source: Eurostat (hlth_silc_10)
In the EU, the gender health gap concerning the share of the population reporting very good or good health was observed for all age groups. In 2022, the gap was lowest for the age group 25–34 years (1.3 percentage points). It ranged between 1.3 and 3.8 percentage points for most of the 10-year age groups but was notably higher for people aged 75–84 years, at 4.8 percentage points.
People with a higher level of educational attainment perceive their health as better…
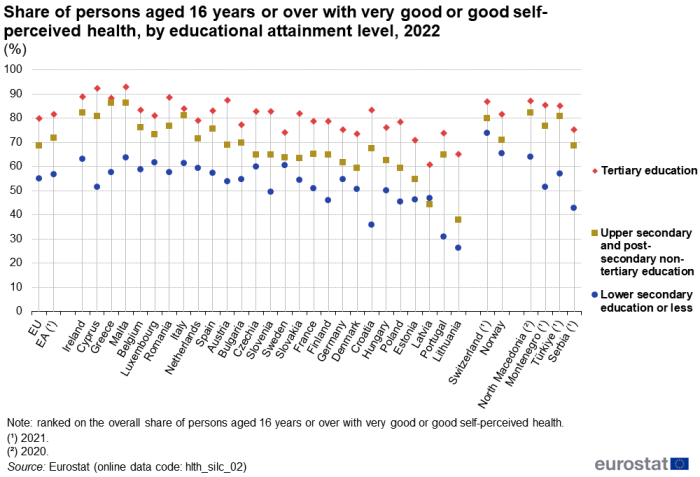
Clear differences appear when looking at the relationship between self-perceived health and educational attainment levels in 2022 – see Figure 3. In the EU, the shares of people aged 16 years or over perceiving their health as very good or good were:
- 55.1 % for people having completed, at most, lower secondary education;
- 68.7 % for people having completed upper secondary or post-secondary non-tertiary education;
- 80.0 % for people having completed tertiary education.
(%)
Source: Eurostat (hlth_silc_02)
A health gap between educational attainment levels is apparent in most of the EU Member States, nearly always with the same pattern as the one observed for the EU as a whole. The only exception was Latvia, where the share of people reporting very good or good health in 2022 was slightly lower for people having completed upper secondary and post-secondary non-tertiary education than for people having completed, at most, lower secondary education.
In 2022, the largest gaps in the share of the population aged 16 years or over reporting very good or good health between those with the highest and the lowest educational attainment levels were observed in Croatia (47.6 percentage points), Portugal (42.9 percentage points) and Cyprus (40.9 percentage points). The smallest gaps were observed in Latvia and Sweden, at 14.0 percentage points and 13.6 percentage points, respectively. Among the non-EU countries for which data are presented in Figure 3, relatively narrow gaps were observed in Norway and Switzerland (2021 data).
… as did people with a higher level of income
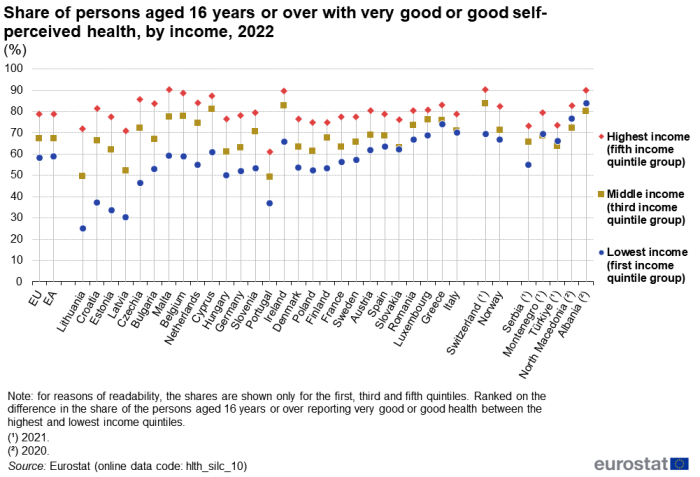
In the EU, 58.2 % of the population aged 16 years or over in the first income quintile (the 20 % of the population with the lowest income) perceived their health as very good or good in 2022. This can be compared with 61.4 % for the second quintile, 67.2 % for the third (middle) quintile, 72.5 % for the fourth quintile and 78.8 % for the fifth (highest) income quintile (the 20 % of the population with the highest income). For reasons of readability, Figure 4 presents the shares for the lowest, middle and highest quintiles only.
(%)
Source: Eurostat (hlth_silc_10)
In 2022, most of the EU Member States showed a similar pattern to that observed for the EU as a whole: the lowest share of people aged 16 years or over who perceived their health as very good or good was recorded for the first income quintile; the share was higher across each higher income quintile; and the highest share was recorded for the fifth income quintile.
- Denmark, Greece, Italy and Slovakia were exceptions, in that the lowest shares of people aged 16 years or over who perceived their health as very good or good was recorded for the second (rather than the first) income quintile.
- Luxembourg was also an exception, in that the share of people aged 16 years or over who perceived their health as very good or good was somewhat lower for the fourth income quintile than for the third income quintile.
The largest differences in the shares of the people aged 16 years or over reporting very good or good health between the subpopulations in the highest and lowest income quintiles were observed in the Baltic Member States and Croatia: in 2022, the differences were 46.7 percentage points in Lithuania, 44.0 percentage points in Croatia, 43.8 percentage points in Estonia and 40.5 percentage points in Latvia; the income health gap was also relatively wide in Czechia (39.5 percentage points). By contrast, relatively little difference was observed between the income groups with the highest and lowest shares in Greece (11.0 percentage points) and Italy (10.6 percentage points); in both cases, the lowest shares were for the second rather than the lowest income group.
Chronic morbidity: long-standing illnesses or health problems
In 2022, more than one third of people in the EU report having a long-standing illness or health problem
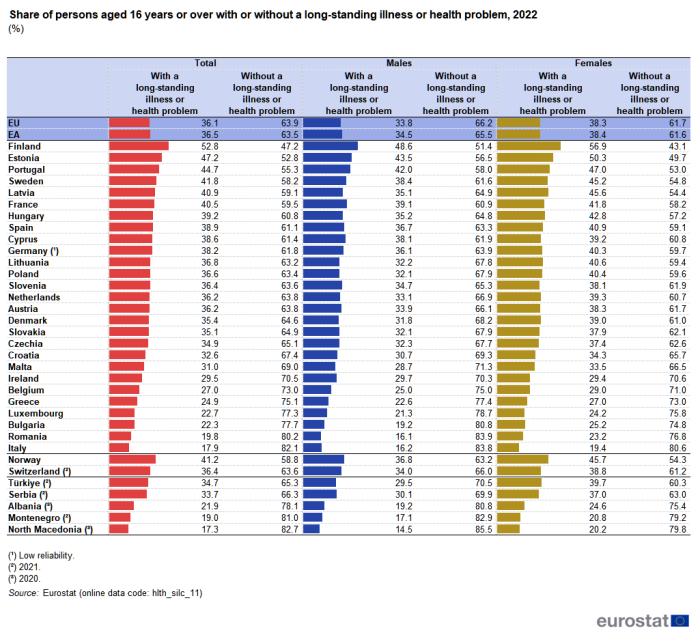
In 2022, 36.1% of the EU population aged 16 years or over reported having a long-standing illness or health problem.
(%)
Source: Eurostat (hlth_silc_11)
Among the EU Member States, the lowest shares of people aged 16 years or over with a long-standing illness or health problem were observed in Italy (17.9 %) and Romania (19.8 %). Among non-EU countries, low shares were also observed in North Macedonia (17.3 %; 2020 data) and Montenegro (19.0 %; 2021 data). Most Member States reported shares ranging between 22.3 % and 44.7 %, with higher shares observed in Estonia (47.2 %) and Finland (52.8 %) – see Table 2.
A long-standing illness or health problem is less common among males than females
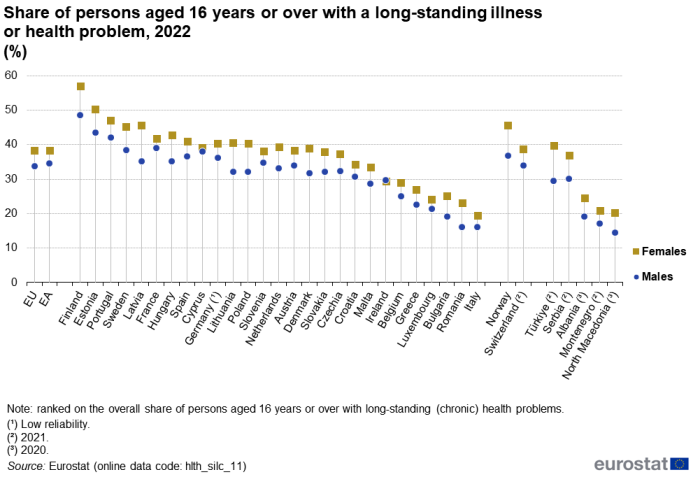
Similar to self-perceived health, a lower share of males than females reported a long-standing illnesses or health problem: in 2022, the share for males in the EU was 33.8 % while the corresponding share for females was 4.5 percentage points higher at 38.3 % – see Figure 5.
(%)
Source: Eurostat (hlth_silc_11)
Across nearly all of the EU Member States, a lower share of males than females reported a long-standing illnesses or health problem in 2022. The widest gender gaps for this indicator were observed in Poland (8.3 percentage points), Finland (also 8.3 percentage points), Lithuania (8.4 percentage points) and Latvia (10.5 percentage points); a relatively wide gap was also observed in Türkiye (10.2 percentage points; 2021 data). The narrowest gaps among the Member States were recorded in Cyprus (1.1 percentage points) and Ireland, where a slightly higher share (0.3 percentage points difference) of males than females reported a long-standing illness or health problem.
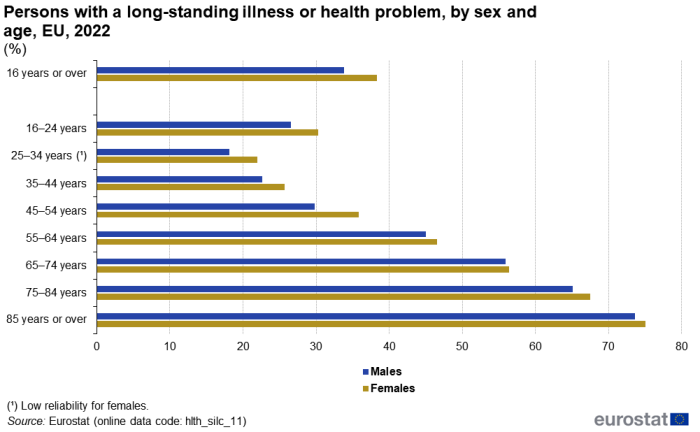
(%)
Source: Eurostat (hlth_silc_11)
A major factor in the prevalence of long-standing illnesses or health problems is age. More than one quarter (28.4 %) of people in the EU aged 16–24 years reported a long-standing illness or health problem in 2022, with this share notably lower among people aged 25–34 years, at 20.0 %. From this age group upwards, there was a fairly regular age gradient, with the prevalence of long-standing illnesses or health problems peaking at close to three quarters (74.5 %) among people aged 85 years and over – see Figure 6.
A smaller share of employed persons report long-standing illness or health problem than unemployed persons
There is also a relationship between working status and the share of people aged 16 years or over with a long-standing illness or health problem – see Figure 7. Whereas slightly more than one quarter (26.0 %) of employed persons in the EU reported such problems in 2022, the share was around two fifths (40.9 %) for unemployed persons.
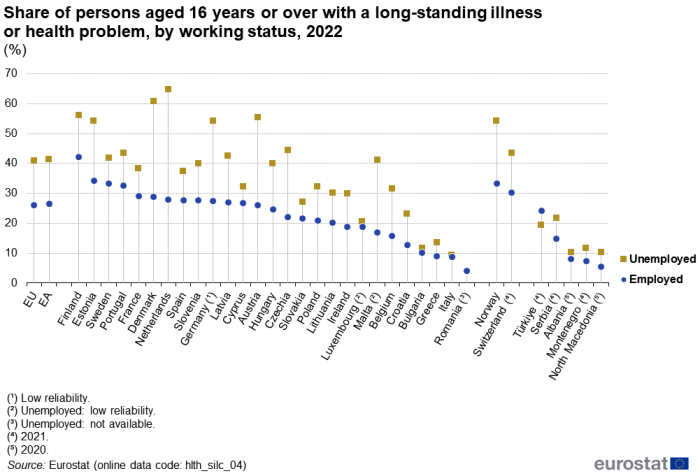
(%)
Source: Eurostat (hlth_silc_04)
All of the EU Member States reported the same overall pattern as described for the EU, with a lower share of persons aged 16 years or over reporting a long-standing illness or health problem among employed persons than among unemployed persons in 2022. In percentage point terms, the largest difference was observed in the Netherlands, as the share for employed persons was 27.9 %, some 36.8 percentage points lower than the share for unemployed persons (64.7 %). The next largest difference was 31.9 percentage points in Denmark, while Austria and Germany (low reliability) were the only other Member States to record a difference of more than 25.0 percentage points. At the other end of the range, the smallest differences were reported in Luxembourg (1.8 percentage points; data for unemployed persons is of low reliability), Bulgaria (1.5 percentage points) and Italy (0.7 percentage points).
Among the non-EU countries shown in Figure 7, Norway also reported a relatively large difference (21.1 percentage points). Türkiye was the only non-EU country for which data are available to have a higher share of persons reporting a long-standing illness or health problem among employed persons than among unemployed persons, with a difference of 4.9 percentage points (2021 data).
Source data for tables and graphs
Data sources
The data used in this article are derived from EU statistics on income and living conditions (EU-SILC). This source provides annual data for the EU Member States as well as most EFTA and enlargement countries on income, poverty, social exclusion and other aspects of living conditions.
The reference population for EU-SILC is limited to private households and their current members residing in the territory of the surveying country at the time of data collection. People living in collective households and institutions are generally excluded from the reference population. All household members are surveyed, but only those aged 16 years or over are interviewed.
The source is documented in more detail in this background article which provides information on the scope of the data, its legal basis, the methodology employed, as well as related concepts and definitions.
Limitations of the data
All of the indicators presented in this article are derived from self-reported data so they are, to a certain extent, affected by respondents’ subjective perception as well as by their social and cultural background. Despite their subjective nature, the statistics that are presented are considered to be relevant and reliable estimators of the health status of populations as well as good predictors of health care needs; they are also valuable for trend analyses and for measuring socioeconomic disparities.
EU-SILC does not cover the institutionalised population, for example, people living in health and social care institutions whose health status is likely to be worse than that of the population living in private households. It is therefore likely that, to some degree, this data source under-estimates the share of the population with health problems. Another factor that may influence the results shown is the different organisation of health care services, be that nationally or locally. Furthermore, the indicators presented are not age-standardised and thus reflect the current national age structures. Finally, despite substantial and continuous efforts for harmonisation, the implementation of EU-SILC is organised nationally, which may impact on the results presented, for example, due to differences in the formulation of questions or their precise coverage.
Context
The World Health Organization defines health as ‘a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity’, which alludes to its multidimensional nature and a range of different indicators for measuring it.
Good health is an asset in itself. It is not only of value to the individual as a major determinant of quality of life, well-being and social participation, but it also contributes to general social and economic growth. Many factors influence the health status of a population and these can be addressed by health and other policies regionally, nationally or across the EU.
Indicators on health status are given high importance in EU health policies. The monitoring of health status of populations was included in the overarching EU strategy Together for Health: A Strategic Approach for the EU 2008–2013 (COM(2007) 630 final) and in the more recent Investing in health working document and the EU4Health programme 2021–2027 – a vision for a healthier European Union.
Health status monitoring is also important for more topical policies such as active and healthy living in the digital world, health inequalities and social protection and social inclusion.
Three general health questions on self-perceived health, chronic morbidity and disability (long-term activity limitation) constitute the minimum European health module (MEHM). Indicators based on these three questions are included in the health status chapter of the European core health indicators (ECHI).
The health status of individuals and of the population in general is determined by a complex set of factors: genetic dispositions, individual behaviour, environmental, cultural and socioeconomic conditions, as well as by the functioning of healthcare services. Eurostat provides data on different health determinants that can help to explain the different levels and distribution of health status among the population, such as:
- health care,
- accidents at work and work-related health problems,
- living conditions and welfare,
- the labour market, in particular unemployment,
- education and training.
Direct access to
Online publications
Health status
- Healthy life years
- Long-term care statistics
- Population with disability
- Mortality and life expectancy
Methodology
General health statistics articles
- Health (hlth), see:
- Health status (hlth_state)
- Self-perceived health and well-being (hlth_sph)
- Self-reported chronic morbidity (hlth_srcm)
- Income and living conditions (ilc) (SIMS metadata file)
- Health variables of EU-SILC (ESMS metadata file – hlth_silc_01_esms)
- EU statistics on income and living conditions (EU-SILC) methodology
- Health variables in EU-SILC
- European Commission – Directorate-General for Health and Public Safety – Public health, see:
- Regulation (EU) 2021/522 of the European Parliament and of the Council of 24 March 2021 establishing a Programme for the Union's action in the field of health (‘EU4Health Programme’) for the period 2021–2027