What is it?
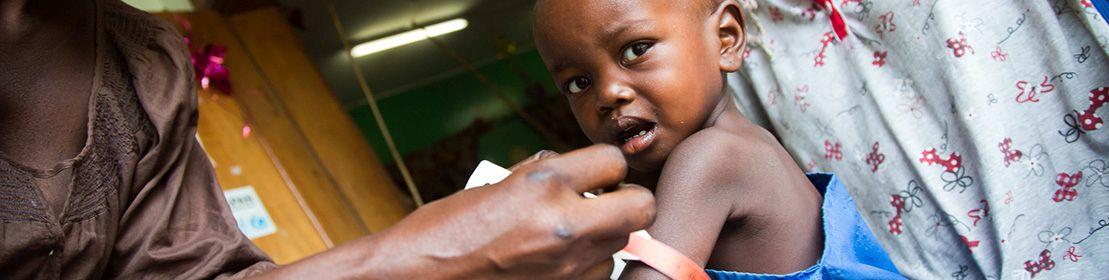
Child undernutrition is a widespread health issue, taking forms such as wasting (low weight-for-height), stunting (low height-for-age), and micronutrient deficiencies. These can all occur simultaneously.
Malnutrition arises from underlying factors such as:
- inadequate dietary intake
- limited access to nutritious food and safe water, poor sanitation, and lack of access to health care and social services
- inadequate childcare
- lack of education.
These factors are often structural, linked to poverty and are exacerbated by disaster, conflict, disease outbreak or forced displacement.
Why is this important?
Child undernutrition is a leading contributor to death and disability globally, and is responsible for nearly half of deaths in children under 5 years old. It weakens immunity and leads to increased frequency and severity of common infections, putting children at risk of delayed recovery and even death.
Illnesses can in turn become a cause of undernutrition in a potentially lethal cycle of worsening illness, deteriorating nutritional status and repeated infections. Therefore, malnutrition must be addressed to tackle diseases such as malaria, diarrhoea, and pneumonia.
Acute undernutrition remains a major concern in humanitarian emergencies and protracted crises. In 2022, over 35 million children under 5 years old suffered from wasting across 30 food crises, according to the 2023 Global Report against Food Crisis.

Malnourishment leads to a higher fatality rates in children: a severely malnourished child is roughly 11 times more likely to die of a common infection than a healthy counterpart.
148.1 million children under 5 years old were affected by stunting globally in 2022 – nearly all in Asia and Africa, according to the WHO and UNICEF Joint Child Malnutrition Estimates 2023. Whilst stunting cannot be treated, it can be prevented by addressing acute undernutrition and implementing nutrition-sensitive approaches.
How are we helping?
The EU is committed to a world free from all forms of malnutrition by 2030.
The EU addresses acute malnutrition through an integrated multi-sectoral approach, combining (i) the assessment of nutritional status of children, (ii) the treatment of acute malnutrition, and (iii) the prevention of all forms of malnutrition.

Treatment
Acute undernutrition, or wasting, results in a high risk of death, despite being both preventable and curable. The Community-based Management of Acute Malnutrition (CMAM) adopted by UNICEF, the WHO and WFP in 2007 has led to a significant transformation in addressing acute malnutrition across 70 countries. However, CMAM’s impact remains limited.
To tackle acute undernutrition in crisis situations, the EU and its humanitarian partners intervene by supporting nutritional programmes. This is increasingly delivered as part of a package of integrated health and nutrition services. In high-risk areas, the EU also strengthens the response capacities and shock responsivity of existing community and health systems.
The EU allocated €200 million to humanitarian nutrition projects in 2022. At the Nutrition for Growth (N4G) Summit in Tokyo 2021, the EU pledged to commit a further €2.5 billion for international assistance.
However, more funding is still needed. We have been implementing programmatic partnerships since 2021. These partnerships include multi-year funding, creating more reliability and facilitating more forward-looking and sustainable programming. For nutrition, several multi-year contracts have been implemented over the last years.
Prevention
While treatment of acute malnutrition is essential to saving lives, it is increasingly clear that the focus should simultaneously be on actions to prevent further suffering.
The EU considers nutrition within all its programming to foster a nutritional impact in humanitarian interventions and reinforce the link between humanitarian and development programming. Effective investment in multi-sectoral approaches to tackle the underlying causes of malnutrition, is therefore essential.
Examples of prevention strategies include:
- food security and livelihood interventions
- the provision of access to safe drinking water and sanitation facilities for affected communities
- free access to healthcare for children and pregnant and lactating mothers.

Innovation
The EU supports innovative and simplified approaches aimed at optimising performance, coverage, and cost-efficiency of treatment protocols.
The EU supports so-called “simplified approaches” that allow the provision of wasting treatment in areas where it would be otherwise impossible, for example by using community health workers.
Other approaches including digitalisation also have a huge role to play and can facilitate both access to and delivery of service, e.g., in determining and monitoring with mobile devices the nutritional condition of beneficiaries.
Last updated: 13/12/2023
Facts & figures
In 2022, over 35 million children under 5 years old suffered from wasting in 30 countries and over 148.1 million were affected by stunting.
The EU allocated over €200 million to humanitarian nutrition projects in 2022.
Related information
- Global Nutrition Report 2020
- Guidance for Programming - Infant and Young Children – Feeding in Emergencies (2014)
- Thematic Policy Document - Nutrition - Addressing Undernutrition in Emergencies (2013)
- Technical Issue Paper - Use of the simplified protocol for treatment of acute undernutrition (2017)
- Technical Issue Paper – Wash and Nutrition (2016)
- Technical Issue Paper - Community-based Management of Acute Malnutrition (CMAM) (2011)
- Technical Issue Paper - Nutritional products and strategy for their use in curative and preventive treatment of Moderate Acute Malnutrition (2009)